“Hello, Listeners. In Breaking News: The Sky. The Earth. Life! Existence As An Unchanging Plane With

“Hello, listeners. In breaking news: the sky. The Earth. Life! Existence as an unchanging plane with horizons of birth and death in the faint distance. We have nothing to speak about. There never was. Words are an unnecessary trouble. Expression is time, wasting away. Any communication is just a yelp in the darkness. Ladies, gentlemen, listeners. You. I am speaking now, but I am saying nothing! I am just making noises and, as it happens, they are organized in words, and you should not draw meaning from this.”
More Posts from Marvelousmellifluousvoice and Others

Your eyes wander up, and above you see the dark planet of awesome size perched, in it’s sunless void. An invisible titan all thick black forests and jagged mountains and deep, turbulent oceans.
A monster. Spinning, soundless, forgotten. It’s so close now. You see it just above you. Maybe, even, if you tried very hard, you could.. touch it. You reach up-

So i choose to stay in the hotel tonight & Lauren takes Cecil & Dylan off to understand the lights above the Arby’s. (omg these two)



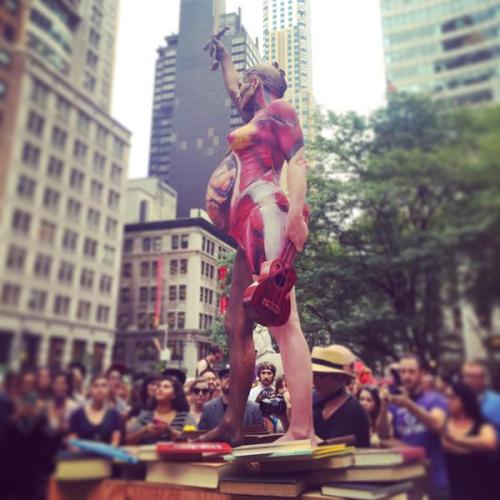




Amanda Palmer as a statue for a children’s book benefit at the New York Public Library.
And here’s David Hirst’s Verity, that she’s recreating.


https://www.youtube.com/embed/9QlDX8mPAcc?feature=oembed
I love Amanda so much. This is an animation that uses a voice memo from her phone of a conversation she had with me while I was asleep (I can have conversations while I am asleep, I am told by people who have tried it).
She found the message she had left for herself on her phone a year or so after she’d left it, and played it to me. I said it sounded like an animated film, and she agreed, and used her Patreon to make it happen…
Only watch it if you want to know what the inside of my head is probably like while I am asleep.
(via https://www.youtube.com/watch?v=9QlDX8mPAcc)

“There were no paved roads here when I was a boy. We had to walk for 3 days to get to places that only take 2 hours now. There was never any money for school. We had no wealth or property. Beginning at six years old, I cleaned dishes at a restaurant until 9 pm. Then I would go to sleep and start again. All my money went to my parents. I’d hear stories about cities and airplanes, but they seemed like fairy tales. I’d dream of visiting these places, but before I could get too far, I’d be hungry again. So I grew up thinking that the entire world was like our valley. I thought all children lived like me. Then one day when I turned 16, I had the opportunity to visit to the city of Gilgit. I couldn’t believe it. I saw a boy eating at a restaurant with his father. He was my age. He was wearing a school uniform. I broke down in tears.” (Hunza Valley, Pakistan)

Sigh










South Dakotan sculptor John Lopez creates life-sized scrap metal sculptures with a uniquely Western American twist. In his hands, old discarded farm equipment is recycled into sculptures of iconic creatures from the American West like a bison, a horse plowing a field, or a Texas Longhorn.
A doctor discovers an important question patients should be asked
This patient isn’t usually mine, but today I’m covering for my partner in our family-practice office, so he has been slipped into my schedule.
Reading his chart, I have an ominous feeling that this visit won’t be simple.
A tall, lanky man with an air of quiet dignity, he is 88. His legs are swollen, and merely talking makes him short of breath.
He suffers from both congestive heart failure and renal failure. It’s a medical Catch-22: When one condition is treated and gets better, the other condition gets worse. His past year has been an endless cycle of medication adjustments carried out by dueling specialists and punctuated by emergency-room visits and hospitalizations.
Hemodialysis would break the medical stalemate, but my patient flatly refuses it. Given his frail health, and the discomfort and inconvenience involved, I can’t blame him.
Now his cardiologist has referred him back to us, his primary-care providers. Why send him here and not to the ER? I wonder fleetingly.
With us is his daughter, who has driven from Philadelphia, an hour away. She seems dutiful but wary, awaiting the clinical wisdom of yet another doctor.
After 30 years of practice, I know that I can’t possibly solve this man’s medical conundrum.
A cardiologist and a nephrologist haven’t been able to help him, I reflect,so how can I? I’m a family doctor, not a magician. I can send him back to the ER, and they’ll admit him to the hospital. But that will just continue the cycle… .
Still, my first instinct is to do something to improve the functioning of his heart and kidneys. I start mulling over the possibilities, knowing all the while that it’s useless to try.
Then I remember a visiting palliative-care physician’s words about caring for the fragile elderly: “We forget to ask patients what they want from their care. What are their goals?”
I pause, then look this frail, dignified man in the eye.
“What are your goals for your care?” I ask. “How can I help you?”
The patient’s desire
My intuition tells me that he, like many patients in their 80s, harbors a fund of hard-won wisdom.
He won’t ask me to fix his kidneys or his heart, I think. He’ll say something noble and poignant: “I’d like to see my great-granddaughter get married next spring,” or “Help me to live long enough so that my wife and I can celebrate our 60th wedding anniversary.”
His daughter, looking tense, also faces her father and waits.
“I would like to be able to walk without falling,” he says. “Falling is horrible.”
This catches me off guard.
That’s all?
But it makes perfect sense. With challenging medical conditions commanding his caregivers’ attention, something as simple as walking is easily overlooked.
A wonderful geriatric nurse practitioner’s words come to mind: “Our goal for younger people is to help them live long and healthy lives; our goal for older patients should be to maximize their function.”
Suddenly I feel that I may be able to help, after all.
“We can order physical therapy — and there’s no need to admit you to the hospital for that,” I suggest, unsure of how this will go over.
He smiles. His daughter sighs with relief.
“He really wants to stay at home,” she says matter-of-factly.
As new as our doctor-patient relationship is, I feel emboldened to tackle the big, unspoken question looming over us.
“I know that you’ve decided against dialysis, and I can understand your decision,” I say. “And with your heart failure getting worse, your health is unlikely to improve.”
He nods.
“We have services designed to help keep you comfortable for whatever time you have left,” I venture. “And you could stay at home.”
Again, his daughter looks relieved. And he seems … well … surprisingly fine with the plan.
I call our hospice service, arranging for a nurse to visit him later today to set up physical therapy and to begin plans to help him to stay comfortable — at home.
Back home
Although I never see him again, over the next few months I sign the order forms faxed by his hospice nurses. I speak once with his granddaughter. It’s somewhat hard on his wife to have him die at home, she says, but he’s adamant that he wants to stay there.
A faxed request for sublingual morphine (used in the terminal stages of dying) prompts me to call to check up on him.
The nurse confirms that he is near death.
I feel a twinge of misgiving: Is his family happy with the process that I set in place? Does our one brief encounter qualify me to be his primary-care provider? Should I visit them all at home?
Two days later, and two months after we first met, I fill out his death certificate.
Looking back, I reflect: He didn’t go back to the hospital, he had no more falls, and he died at home, which is what he wanted. But I wonder if his wife felt the same.
Several months later, a new name appears on my patient schedule: It’s his wife.
“My family all thought I should see you,” she explains.
She, too, is in her late 80s and frail, but independent and mentally sharp. Yes, she is grieving the loss of her husband, and she’s lost some weight. No, she isn’t depressed. Her husband died peacefully at home, and it felt like the right thing for everyone.
“He liked you,” she says.She’s suffering from fatigue and anemia. About a year ago, a hematologist diagnosed her with myelodysplasia (a bone marrow failure, often terminal). But six months back, she stopped going for medical care.
I ask why.
“They were just doing more and more tests,” she says. “And I wasn’t getting any better.”
Now I know what to do. I look her in the eye and ask:
“What are your goals for your care, and how can I help you?”
-Mitch Kaminski
Source

Your Horoscopes — Week Of August 4, 2015
-
 thousand-winters reblogged this · 2 weeks ago
thousand-winters reblogged this · 2 weeks ago -
 killingkueen reblogged this · 1 month ago
killingkueen reblogged this · 1 month ago -
 devin-the-writes reblogged this · 1 month ago
devin-the-writes reblogged this · 1 month ago -
 friedeggfarmmuffin liked this · 2 months ago
friedeggfarmmuffin liked this · 2 months ago -
 theclownfromdowntown liked this · 2 months ago
theclownfromdowntown liked this · 2 months ago -
 caffeinated-emo-twink liked this · 2 months ago
caffeinated-emo-twink liked this · 2 months ago -
 just-ghost-ghosting-around liked this · 2 months ago
just-ghost-ghosting-around liked this · 2 months ago -
 autisticrodent liked this · 2 months ago
autisticrodent liked this · 2 months ago -
 geek-academique liked this · 2 months ago
geek-academique liked this · 2 months ago -
 dysphoria-things reblogged this · 2 months ago
dysphoria-things reblogged this · 2 months ago -
 dysphoria-things liked this · 2 months ago
dysphoria-things liked this · 2 months ago -
 fearforthestorm reblogged this · 2 months ago
fearforthestorm reblogged this · 2 months ago -
 goingtobeamazing reblogged this · 2 months ago
goingtobeamazing reblogged this · 2 months ago -
 thousand-winters liked this · 2 months ago
thousand-winters liked this · 2 months ago -
 fazmid liked this · 2 months ago
fazmid liked this · 2 months ago -
 another-dead-intern reblogged this · 2 months ago
another-dead-intern reblogged this · 2 months ago -
 luckyicekitsune liked this · 2 years ago
luckyicekitsune liked this · 2 years ago -
 crystalline-kaleidoscope reblogged this · 3 years ago
crystalline-kaleidoscope reblogged this · 3 years ago -
 tsukiyakibowl liked this · 4 years ago
tsukiyakibowl liked this · 4 years ago -
 capricornfraud liked this · 4 years ago
capricornfraud liked this · 4 years ago -
 datmoongamer reblogged this · 5 years ago
datmoongamer reblogged this · 5 years ago -
 datmoongamer liked this · 5 years ago
datmoongamer liked this · 5 years ago -
 ritathememermaid liked this · 5 years ago
ritathememermaid liked this · 5 years ago -
 bleedingnoses reblogged this · 5 years ago
bleedingnoses reblogged this · 5 years ago -
 crayonhyacinth liked this · 5 years ago
crayonhyacinth liked this · 5 years ago -
 eelshell liked this · 5 years ago
eelshell liked this · 5 years ago -
 storekn1fe liked this · 5 years ago
storekn1fe liked this · 5 years ago -
 owl-bathrobe reblogged this · 6 years ago
owl-bathrobe reblogged this · 6 years ago -
 seabhacs liked this · 6 years ago
seabhacs liked this · 6 years ago -
 cheslan liked this · 6 years ago
cheslan liked this · 6 years ago -
 theunknownteen reblogged this · 6 years ago
theunknownteen reblogged this · 6 years ago -
 theunknownteen liked this · 6 years ago
theunknownteen liked this · 6 years ago -
 namaaz liked this · 6 years ago
namaaz liked this · 6 years ago -
 souriise liked this · 6 years ago
souriise liked this · 6 years ago -
 lanternrayner liked this · 6 years ago
lanternrayner liked this · 6 years ago -
 wonder-marvel liked this · 6 years ago
wonder-marvel liked this · 6 years ago -
 taddy-mason liked this · 6 years ago
taddy-mason liked this · 6 years ago -
 bloodylady003 liked this · 6 years ago
bloodylady003 liked this · 6 years ago -
 kler-dr-blog liked this · 6 years ago
kler-dr-blog liked this · 6 years ago -
 grandsharkaliengarden-blog liked this · 6 years ago
grandsharkaliengarden-blog liked this · 6 years ago -
 dowagerking liked this · 7 years ago
dowagerking liked this · 7 years ago -
 froggy99sworld reblogged this · 7 years ago
froggy99sworld reblogged this · 7 years ago -
 froggy99sworld liked this · 7 years ago
froggy99sworld liked this · 7 years ago -
 isabelless123-blog liked this · 7 years ago
isabelless123-blog liked this · 7 years ago -
 virginiangingerplant reblogged this · 7 years ago
virginiangingerplant reblogged this · 7 years ago -
 murderfun reblogged this · 7 years ago
murderfun reblogged this · 7 years ago -
 blushbite liked this · 7 years ago
blushbite liked this · 7 years ago -
 whatsocialliferambles liked this · 7 years ago
whatsocialliferambles liked this · 7 years ago -
 themadnesslovesu143 liked this · 7 years ago
themadnesslovesu143 liked this · 7 years ago -
 cryptidculture reblogged this · 7 years ago
cryptidculture reblogged this · 7 years ago
Things I like! Quotes from classic literature, nature, photography, other art- especially Vincent van Gogh, archery, and Welcome to Night Vale.
91 posts

